In a paper published in Ecological Economics, researchers explore the different components that need to be addressed when assessing the sustainability of antimicrobial use (AMU) in animal agriculture. Photo: J. Lokrantz/Azote
Bildtext får vara max två rader text. Hela texten ska högerjusteras om den bara ska innehålla fotobyline! Photo: B. Christensen/Azote
ANTIMICROBIAL USE AND RESISTENCE
Antimicrobial farm
New study proposes how to asses the sustainability of antimicrobial use in animal agriculture and how to regulate it on a global scale. For the sake of both human and animal health
- Society faces a trade-off between using antimicrobials in farm animals and risking public health as antimicrobial use leads to drug resistant microbes that are difficult to treat.
- The authors take a closer look at what drive, push and ultimately lead to antimicrobial use and resistance.
- They propose a set of indicators that they believe can capture the social, environmental, and economic implications of both the use and the resistance to antimicrobials.
When it comes to our connections with farm animals, the consumption of them are about as close as it gets. Thus animals’ health impacts meat eaters’ health.
Antimicrobial resistance (AMR) in humans, the unintended consequence of using antimicrobials in farm animals, is a growing public health concern.
It creates the problem of multi-drug resistant diseases that are almost impossible to treat. This is why growth promoters have now been banned in many countries.
But other antimicrobials continue to be used given their benefits for animal health and welfare.
Assessing the sustainability of its use is a necessary albeit complex task. In a paper published in Ecological Economics, centre researcher Peter Søgaard Jørgensen along with researchers from Cornell University and the University of Geneva, explore the different components that need to be addressed when assessing the sustainability of antimicrobial use (AMU) in animal agriculture.
Guillaume Lhermie at the College of Veterinary Medicine at Cornell University was lead author.
All things intertwined
The decision to use antimicrobials is dependent on a mix of economic, behavioural, ethical and cultural factors. This is the reason why the researchers take a social-ecological systems (SES) perspective on it. SES can be understood as a system in which human and nature relationships are deeply intertwined with each other.
As lead author Lhermie explains, "In our study, SES can be defined as systems where public health, farming economy, and social issues are intertwined with the animals’ health and welfare issues along with the health and services provided by microorganisms."
In the article the authors take a closer look at what drives and pushes and ultimately leads to anti-microbial use and resistance. This makes it easier to explain how responses to tackle AMR can differ based on what drivers exist.
Responding to system change
While existing models work well when describing the AMU and AMR issue, their usefulness in analysing it from a sustainability policy standpoint is limited.
Søgaard Jørgensen says: “We felt a need to implement a slight move from the descriptive model to an analysis of a continuum of actions. This requires a better understanding of the interactions and interdependencies among economic, social and environmental spheres.”
A sustainability assessment framework of AMU, the goal of the authors here, requires setting boundaries of the system in which the assessment is pursued and defining accurate indicators. It also requires negotiating between a variety of moral, temporal and spatial considerations when making policies.
For instance, a major difficulty with AMU-AMR SES is that although it is possible to set boundaries to AMU exchanges, no geographic boundaries can contain the spread of antimicrobial resistance.
That is what recently happened when in 2008 a conferring resistance to a group of last-resort antibiotic called Carbapenems was discovered in Sweden, thought to have spread from New Dehli in India to the rest of the world.
Essentially, the authors argue, coordinating policy to address human and animal health and food safety and security has to happen at a global scale.
To do so, they propose a set of indicators that they believe can capture the social, environmental, and economic implications of both the use and the resistance to anti-microbes.
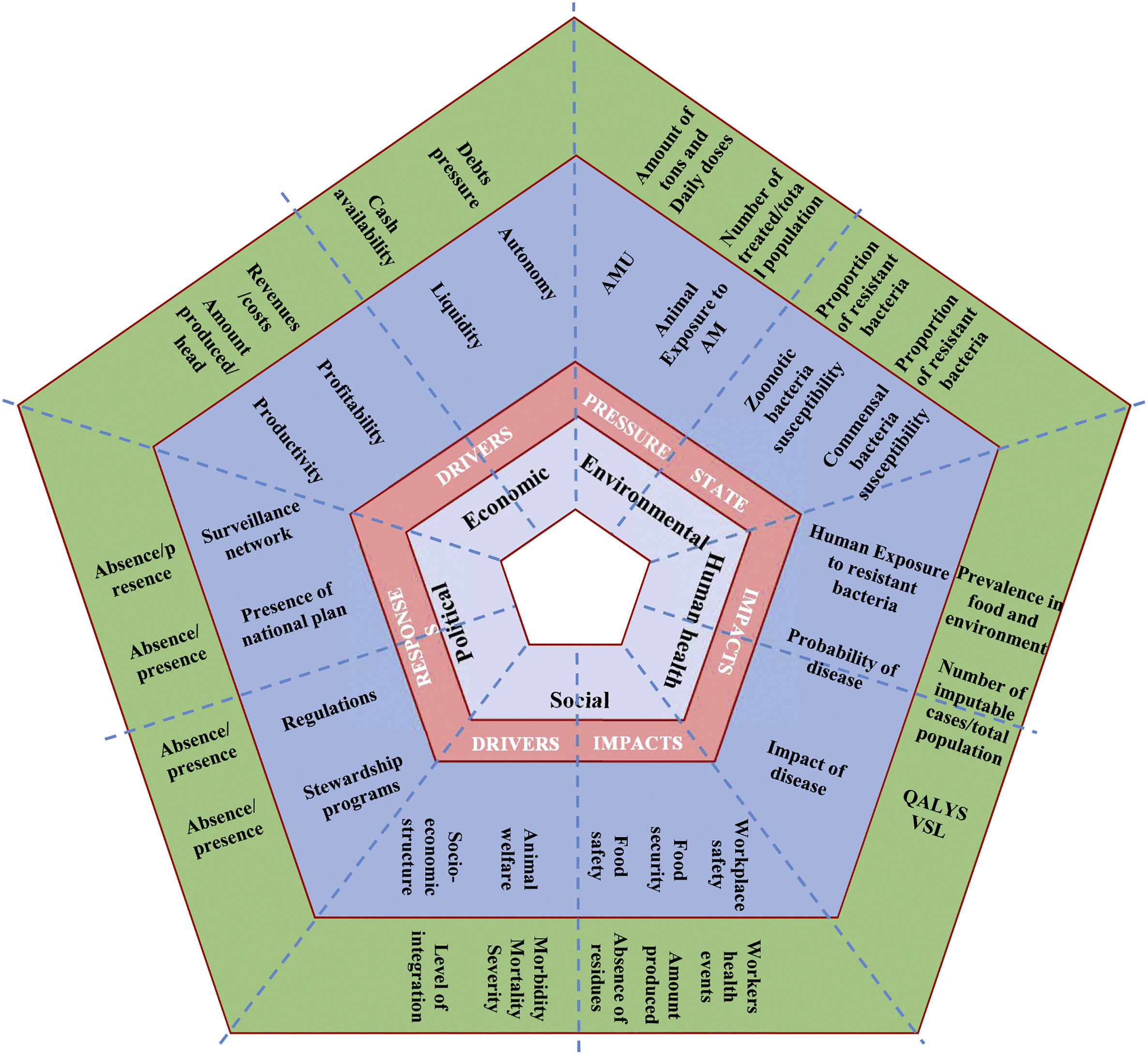
Pentagon of proposed indicators to be assessed. At the center of the pentagon (pale and dark blue), indicators are presented by categories, and superposed to the Driver-Pressure-State-Impact-Response model (pink part). In the green part of the figure, we propose more specific indicators, based on their availability and accuracy. AM: antimicrobials; AMU: antimicrobial use; QALYS: Quality-Adjusted Life Year; VSL: Value of a Statistical Life. Click on illustration to access scientific study.
Getting to better health outcomes
As a final step, Søgaard Jørgensen and colleagues offer two analytical methods that they believe are suitable to assessing AMU when incorporating all indicators shown above. The first one comprises the use of dynamic models to perform cost-benefit analyses. The second consists using multi-criteria decision analysis, which has the advantage of being able to consider both quantitative and qualitative data.
While the complexity of the AMU-AMR SES ecosystem is evident, what is also clear is the necessity to design robust policies that can govern antimicrobial use.
“Given the global mobility of microbes and the uncertainty of the impacts they have on drug resistance, getting AMU regulations right can create huge benefits for human and animal health,” Søgaard Jørgensen and his colleagues conclude.
Rethink Talks: Pandemics, health and global change: how are they connected?
What is the connection between environmental change and diseases such as coronaviruses? How strong is this connection, can we really blame bats, and what does the future of disease risks look like?
Watch conversation with Victor Galaz, deputy director of the Stockholm Resilience Centre, professor Kate Jones from University College London and Peter Søgaard Jørgensen from the Royal Swedish Academy of Sciences, and the Stockholm Resilience Centre.
Lhermie, G., Wernli, D., Jørgensen, P.S, et.al. 2019. Tradeoffs between resistance to antimicrobials in public health and their use in agriculture: Moving towards sustainability assessment. Ecological Economics Volume 166, December 2019, 106427